

Actinic keratosis, also known as solar keratosis or sometimes “sunspots”, is a precancerous skin condition. With this skin condition, lesions (abnormal spots) or actinic keratoses form as a result of overexposure to the sun. Consequently, these lesions typically appear as areas of rough, scaly or crusty skin on the most sun-exposed parts of the body.1,2,3
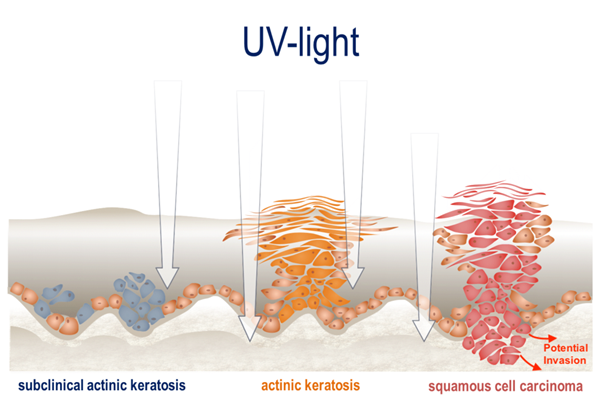
Actinic keratosis develops in the top skin layer that receives the most UV radiation. Therefore, lesions appear most commonly on exposed parts such as the head, face, neck, forearms or backs of the hands.
These lesions may typically: 3,5
A) Appear as flat patches on the face, head and neck.
B) Appear as bumps on the arms and hands.
C) Look pink, red, tan or brown, dark or light, or more than one of these colours.
D) Have a crust or scale that feels dry, rough or horny.
E) Feel itchy.
F) Feel sore, tender or “prickly”.
G) Come and go, usually after sun exposure.
H) Range in size from 1-6 mm, but can grow to several centimetres wide.
I) Occur as several lesions together.
J) Have red, irritated surrounding skin.
K) Appear on the lips (actinic cheilitis), causing dry, scaly or rough textures, cracked lips or loss of colour.
Consult your doctor without delay if you suspect you have symptoms of actinic keratosis. And especially if you notice any of the following: 1,2,4
1) New lesions develop.
2) The patch changes colour.
3) Patches feel tender or painful.
4) The patch develops into a lump.
5) Lesions or scaly spots persist.
6) Any of the lesions become bigger.
7) Lesions bleed.
Actinic keratosis is diagnosed through skin examination, often using a bright light or magnifying lens.
If your doctor suspects a lesion might be cancerous, a skin sample will be taken and analysed in the lab (biopsied).5
Actinic keratosis may be unsightly and sometimes uncomfortable. But most importantly, if this skin condition remains untreated, it can develop into a type of skin cancer – squamous cell carcinoma. This can grow into deeper layers of skin, spread to other parts of the body and potentially be disfiguring and even deadly. While most cases of squamous cell carcinoma are successfully treated, it is far preferable to manage actinic keratosis while it is still in the precancerous stage.6
The good news is that most cases can be effectively and easily treated. Different treatment options are available to destroy or remove the lesions while limiting scarring as much as possible.5
For instance, treatment methods such as cryotherapy (freezing the tissue to destroy it) are effective in removing visible lesions. However, actinic keratosis is a visible indication of a larger sun-damaged area that also includes invisible damage under or around the lesion. This is associated with the risk of it progressing to cancer.
Treatments that only remove visible lesions have higher recurrence rates as the untreated invisible damage becomes visible over time, creating the need for repeated treatments5,7 On the other hand, studies have shown that treatment with topical Imiquimod creams removes both the visible lesions and the invisible damage.7
These creams work by stimulating your immune system to recognise and destroy the abnormal skin cells. Most importantly, they can be used in patients who have single or multiple lesions, as well as in immunocompromised patients.7
Moreover, some therapies, such as cryotherapy, may leave the skin looking damaged after treatment. However, with Imiquimod cream, better skin appearance has been reported post-treatment.8
In addition to its proven efficacy and cosmetic advantages, Imiquimod Cream has a simple regimen and easy self-application. This makes it patients’ preferred choice.
Take the following actions to avoid developing actinic keratosis: 1,2,3,5
1) Limit time in the sun, especially between 10:00 and 14:00.
2) Avoid getting suntanned or sunburned.
3) Wear sun-safe clothes – tightly woven fabrics, broad-brimmed hats, and UV protective sunglasses.
4) Apply sunscreen at least 15 minutes before sun exposure, even on cloudy days, before spending time outdoors. Choose broad-spectrum, water-resistant sunscreens with a sun protection factor (SPF) of at least 30.
5) Protect your lips with SPF lip balm.
6) Don’t use tanning beds and lamps. UV exposure from these can be just as damaging as from the sun.
7) Examine your skin regularly for new lesions or patches. Also, check for changes to existing birthmarks, freckles, moles and bumps. Report any skin changes to your doctor.
8) Discuss your risk profile and how often you need skin check-ups with your doctor. For example, if you’ve already had actinic keratosis, you are at increased risk for developing new lesions and may need more frequent check-ups.
Read more on Basal Cell Carcinoma.




Disclaimer
This e-brochure has been auto-translated for your convenience. While machine translations are helpful, they may contain errors. Medinformer is actively working to have all translations reviewed by professional, mother-tongue language speakers, though this process will take time. For the most accurate information, please refer to the original English version. Medinformer and its partners cannot be held responsible for any inaccuracies that may result from the translation.
Thank you for your understanding.